Breast Reconstruction: Rebuilding After Breast Cancer
What is Breast Reconstruction?
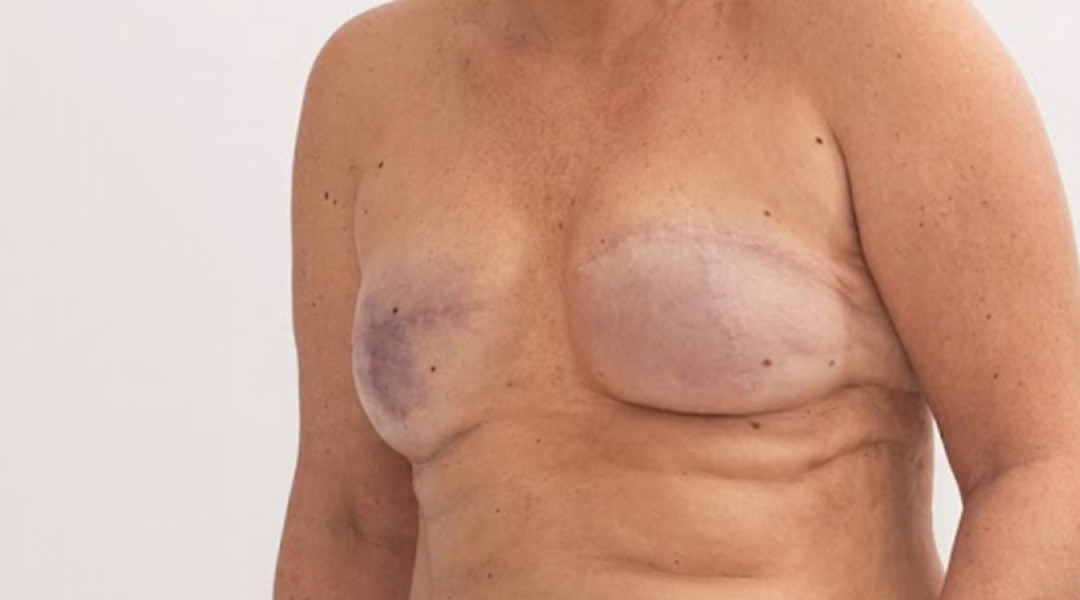
Following a mastectomy (complete removal of the breast) due to breast cancer or surgeries requiring extensive tissue removal, a significant loss in breast form may occur. Breast reconstruction aims to rebuild the lost breast tissue, not for aesthetic enlargement, but as a reconstructive approach that serves as a continuation of cancer treatment.
The goal is to create a breast form suitable for the individual's body proportions, improve balance in clothing, support daily comfort, and help restore body image. The reconstruction plan is evaluated individually, in harmony with the oncological treatment process.
Who is Eligible for Breast Reconstruction?
Breast reconstruction is an option for most patients. However, the questions of "which method" and "when" are answered differently for everyone. Therefore, the decision is made by evaluating disease characteristics, additional treatments (especially radiotherapy), general health, and expectations.
Key Evaluation Factors
• Necessity of radiotherapy
• Comorbidities like diabetes or circulatory issues
• Smoking (affects healing, especially in tissue-based repairs)
• Body structure and available donor sites
• Previous surgeries and tissue quality
When is Breast Reconstruction Performed?
Timing in breast reconstruction is often one of the most critical parts of the treatment. Planning is not about the "now" or "later" dilemma, but rather prioritizing compatibility with cancer treatment and safety.
1) Immediate Reconstruction
Repair begins during the same surgery as the mastectomy. This can offer psychological and aesthetic advantages for some patients, but it is not suitable for everyone; additional treatment plans and tissue conditions are decisive factors.
2) Delayed Reconstruction
Reconstruction is planned after cancer treatments are completed. This is often preferred if radiotherapy is anticipated or if there are conditions affecting tissue healing.
3) Staged Approach
In some patients, reconstruction is performed in planned stages rather than a "one-off procedure." For example, temporary preparation may be done, followed by final shaping later. The aim is to choose the most suitable and safest path for the treatment process.
What are Breast Reconstruction Methods?
The choice of method depends on the breast skin, muscle structure, radiotherapy plan, and the desired outcome. There are generally two main approaches:
Implant-Based Reconstruction
In this approach, the breast form is recreated with an implant. It can be applied in a single session for some patients, while for others, the process progresses in stages with a tissue expander.
What is a Tissue Expander?
A tissue expander is a temporary material placed to expand skin and soft tissue in a controlled manner. Once the appropriate stage is reached, the expander is removed and the reconstruction is completed with a permanent implant.
Why is Special Planning Required with Radiotherapy?
Radiotherapy can cause stiffness, loss of elasticity in the skin and soft tissues, and changes in healing dynamics. Therefore, implant choice, timing, and alternative methods are evaluated more carefully in these cases.
Autologous (Tissue/Flap) Reconstruction
In this method, the breast is recreated using tissue taken from another part of the body. The main goal here is to provide a more natural tissue feel and, in some patients, reduce the need for implants.
Which Donor Areas Can Be Used?
Planning varies according to the patient's body structure. Frequently evaluated areas include:
• Abdominal tissue (techniques such as "DIEP/TRAM")
• Back tissue (can also be planned in combination with an implant)
• Thighs or other areas (in selected cases)
The suitability of these options is determined based on tissue quality, vascular structure, surgical history, and additional treatment plans.
Nipple (Areola) and Symmetry Adjustments
Depending on the type of mastectomy, the nipple may be preserved in some patients, while in others, the nipple and areola can be recreated at a second stage. Additionally, in unilateral reconstructions, extra adjustments can be planned for the opposite breast to ensure balance.
What is the Recovery Process Like?
Recovery time varies depending on the chosen method, whether it is single-stage or staged, and additional treatments. In general, edema, sensitivity, and movement restriction can be seen in the early period. Using a medical bra, wound care, and regular controls as recommended by the doctor directly affect the quality of healing.
Breast Reconstruction is Personalized and Integrated with Treatment
Breast reconstruction is a reconstructive approach aiming to recreate the breast form lost after cancer treatment. Proper method and timing determine both safety and long-term satisfaction. Therefore, the healthiest step is to create a reconstruction plan suitable for personal conditions through a medical examination.
Informational Note: This content is for general informational purposes. Diagnosis and treatment plans are determined through individual medical evaluation.
